PSMA PET Imaging:
Transforming Prostate Cancer Detection and Treatment
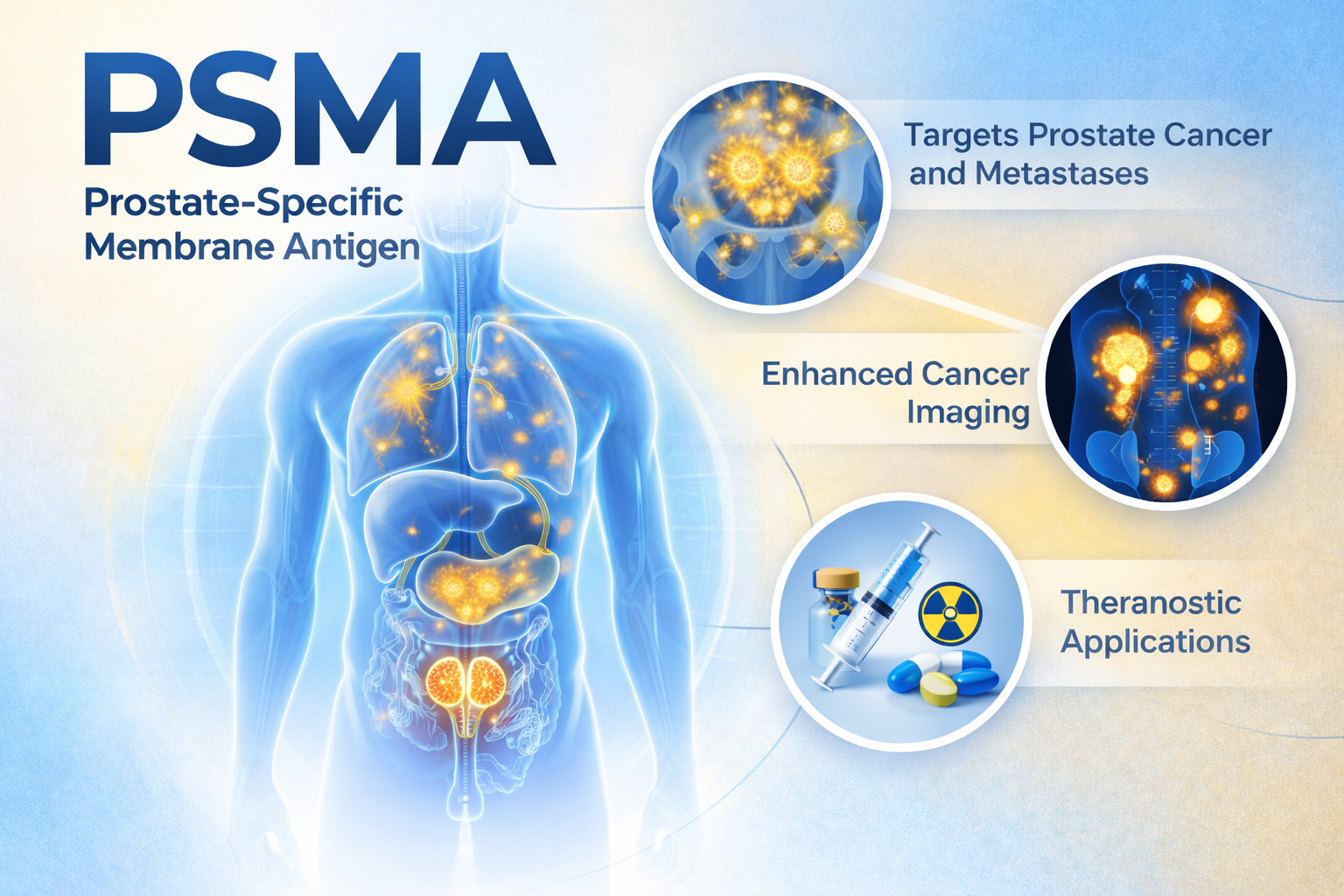
Prostate cancer care has entered a new era with the introduction of PSMA PET imaging—a highly sensitive technique that can detect prostate cancer throughout the body with remarkable accuracy.
Unlike conventional imaging or tracers such as FDG, which highlight glucose metabolism, PSMA PET is specifically designed for prostate cancer. It targets prostate-specific membrane antigen (PSMA), a protein abundantly expressed on prostate cancer cells, especially in advanced and metastatic disease.
How PSMA PET Imaging Works
PSMA PET imaging uses a small amount of a radioactive tracer that is injected into the bloodstream. This tracer is designed to seek out and attach to PSMA on prostate cancer cells.
Once administered, the tracer circulates through the body and binds to areas where prostate cancer is present. The PET scanner then detects the emitted signal and generates detailed images, highlighting even small or otherwise hidden cancer deposits.
To improve anatomical detail, PSMA PET is often combined with CT or MRI, allowing clinicians to pinpoint the exact location of disease within the body.
Types of PSMA PET Imaging
While the principle remains the same, PSMA PET can vary depending on:
- Radionuclide used: Common options include Gallium-68 and Fluorine-18, which differ in production and imaging characteristics.
- Ligands: Molecules such as PSMA-11, piflufolastat, and others that bind specifically to PSMA
- Hybrid imaging systems: Typically PET/CT, with PET/MRI emerging in advanced centers
These variations allow flexibility depending on clinical needs and available infrastructure.
When is PSMA PET Used?
While the principle remains the same, PSMA PET can vary depending on:
- Radionuclide used: Common options include Gallium-68 and Fluorine-18, which differ in production and imaging characteristics.
- Ligands: Molecules such as PSMA-11, piflufolastat, and others that bind specifically to PSMA
- Hybrid imaging systems: Typically PET/CT, with PET/MRI emerging in advanced centers
These variations allow flexibility depending on clinical needs and available infrastructure.
When is PSMA PET Used?
PSMA PET imaging plays a critical role in several stages of prostate cancer management:
In patients with higher-risk disease, PSMA PET can detect whether cancer has spread beyond the prostate (metastatic disease), supporting accurate staging from the outset.
One of its most powerful applications is identifying recurrent prostate cancer, often when PSA levels begin to rise after treatment. It can locate disease even at very low PSA levels, where conventional imaging may fail.
PSMA PET helps map the full extent of disease in patients with metastatic prostate cancer, guiding treatment decisions and monitoring progression.
Clinical Advantages
PSMA PET imaging offers several key benefits:
- High sensitivity and specificity for prostate cancer detection
- Ability to detect disease early and at low PSA levels
- Whole-body imaging, capturing both local and distant disease
- Improved accuracy compared to many conventional imaging methods
- Streamlined imaging process with minimal preparation
These advantages make it a powerful tool for precision diagnosis and treatment planning.
PSMA and Theranostics: Linking Diagnosis and Treatment
PSMA is at the forefront of theranostics—a personalized approach where the same biological target is used for both imaging and therapy.
If PSMA PET imaging shows strong tracer uptake in cancer cells, patients may be eligible for PSMA-targeted radionuclide therapy. In this approach, a therapeutic agent uses the same targeting mechanism to deliver radiation directly to cancer cells, minimizing damage to surrounding healthy tissue.
This allows clinicians to:
- Select patients who are most likely to benefit from therapy
- Deliver targeted treatment based on imaging findings
- Monitor response using the same PSMA pathway
Theranostics represents a major step toward individualized cancer care, where diagnosis and treatment are closely integrated.
Author